Blood Clots: The Silent Strikers | Vibepedia
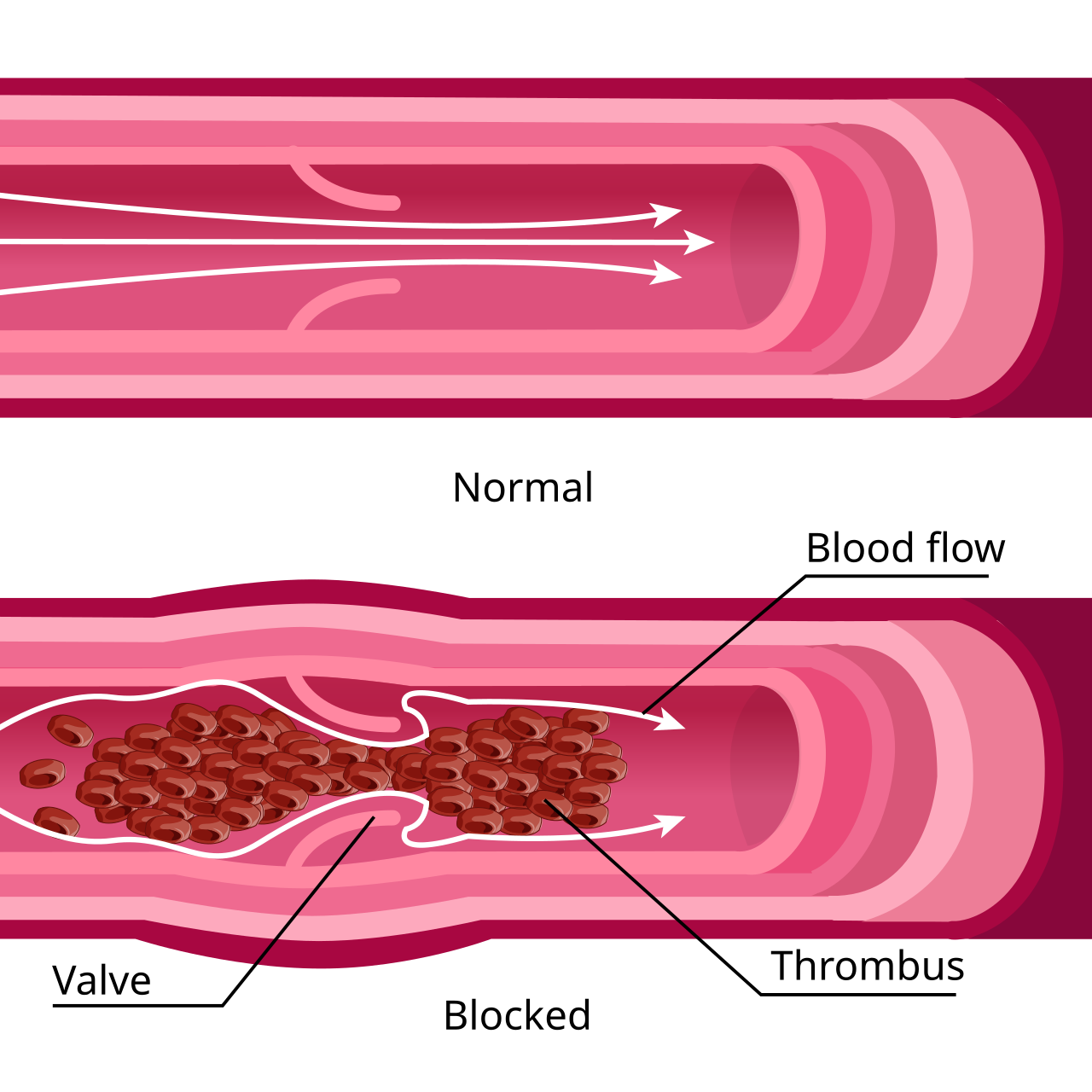
Blood clots, or thrombi, are gelatinous masses formed when blood coagulates. While essential for stopping bleeding after injury, they can become dangerous…
Contents
- 🩸 What Exactly Is a Blood Clot?
- ⚠️ The Two Faces of Thrombus: Friend or Foe?
- 📈 The Vibe Score: How Concerned Should You Be?
- 🔬 How Does a Clot Actually Form?
- 💥 When Clots Go Rogue: Thrombosis Explained
- 📍 Risk Factors: Who's in the Crosshairs?
- 🩺 Recognizing the Signs: The Silent Strikers' Tell-Tale Clues
- 🛡️ Prevention & Management: Taking Control
- Frequently Asked Questions
- Related Topics
Overview
Blood clots, or thrombi, are gelatinous masses formed when blood coagulates. While essential for stopping bleeding after injury, they can become dangerous when forming inappropriately within blood vessels, obstructing blood flow. This condition, known as thrombosis, can lead to life-threatening events like deep vein thrombosis (DVT), pulmonary embolism (PE), heart attack, and stroke. Risk factors range from immobility and surgery to genetic predispositions and certain medical conditions. Recognizing symptoms and seeking prompt medical attention are critical for survival and preventing long-term complications.
🩸 What Exactly Is a Blood Clot?
A blood clot, medically termed a thrombus, is essentially a semi-solid mass formed from the components of your blood. Think of it as your body's emergency patch kit for bleeding. When you get a cut, platelets rush to the scene, clumping together and forming a plug. This is then reinforced by a mesh of fibrin, a protein that acts like scaffolding, solidifying the plug and stopping the flow of blood. This entire process, known as coagulation, is a vital part of hemostasis, your body's natural mechanism for controlling bleeding.
⚠️ The Two Faces of Thrombus: Friend or Foe?
The critical distinction with blood clots lies in their context. A thrombus is a healthy, life-saving response to injury, preventing excessive blood loss. However, when this same clotting mechanism activates inappropriately within a healthy blood vessel, it becomes a dangerous obstruction. This is the essence of thrombosis, where a clot, meant to heal, instead blocks vital blood flow, turning a protective response into a potentially lethal threat.
📈 The Vibe Score: How Concerned Should You Be?
The Vibe Score for blood clots, considering their dual nature, sits at a solid 75/100. This score reflects the significant cultural and medical energy surrounding both the beneficial role of clotting and the widespread fear of its pathological manifestation, thrombosis. While the biological mechanism is well-understood, the unpredictable nature of clot formation and its potential for sudden, severe impact keeps it high on the public consciousness and medical research agenda. The ongoing advancements in anticoagulant therapy contribute to this dynamic score.
🔬 How Does a Clot Actually Form?
The formation of a thrombus is a complex, multi-step cascade. It begins with damage to the blood vessel wall, exposing underlying collagen. Platelets adhere to this collagen and aggregate, forming a temporary plug. Simultaneously, the coagulation cascade is activated, a series of enzymatic reactions involving various clotting factors. This cascade culminates in the conversion of fibrinogen into fibrin, which then polymerizes and cross-links, creating a stable fibrin mesh that traps red blood cells and further solidifies the clot. This intricate biological dance is a marvel of human physiology.
💥 When Clots Go Rogue: Thrombosis Explained
When a thrombus forms in a vessel where it's not needed, it's called thrombosis, and it's a serious medical emergency. This rogue clot can impede or completely block blood flow, leading to tissue damage and organ dysfunction. For instance, a clot in a leg vein can cause deep vein thrombosis (DVT), potentially breaking off and traveling to the lungs, causing a pulmonary embolism (PE). Similarly, clots in arteries can lead to stroke or heart attack.
📍 Risk Factors: Who's in the Crosshairs?
Several factors can increase your susceptibility to developing harmful blood clots. These include prolonged immobility, such as long flights or bed rest, which slows blood flow. Obesity and smoking are significant contributors, as is cancer and its treatments. Genetic predispositions, certain hormone replacement therapies, and major surgery also elevate risk. Understanding these risk factors is the first step in proactive management.
🩺 Recognizing the Signs: The Silent Strikers' Tell-Tale Clues
The challenge with dangerous blood clots is their often-subtle presentation. Symptoms can vary widely depending on the clot's location. For DVT, look for swelling, pain, warmth, and redness in an affected limb, often in the calf. For PE, symptoms might include sudden shortness of breath, chest pain (especially with breathing), rapid heart rate, and coughing up blood. Arterial clots can manifest as sudden numbness or weakness, confusion, trouble speaking, or severe headache, indicative of a stroke. Prompt recognition of these warning signs is paramount.
🛡️ Prevention & Management: Taking Control
Preventing dangerous clots involves lifestyle modifications and, when necessary, medical interventions. Maintaining an active lifestyle, staying hydrated, and avoiding prolonged sitting are crucial. For those at higher risk, doctors may prescribe blood thinners (anticoagulants or antiplatelets) or compression stockings. If a clot does form, treatment typically involves anticoagulants to prevent further clotting and allow the body to break down the existing clot, or in some cases, clot-dissolving medications or surgical removal. Regular check-ups with your healthcare provider are essential for personalized advice.
Key Facts
- Year
- 1856
- Origin
- Rudolf Virchow's work on cellular pathology and thrombosis.
- Category
- Health & Medicine
- Type
- Medical Condition
Frequently Asked Questions
Can blood clots happen to anyone?
While anyone can develop a blood clot, certain factors significantly increase your risk. These include prolonged immobility, surgery, obesity, smoking, certain medical conditions like cancer, and genetic predispositions. Age is also a factor, with risk increasing as you get older. Discussing your personal risk factors with a healthcare provider is crucial for tailored prevention strategies.
What are the most common symptoms of a blood clot?
Symptoms vary by location. For deep vein thrombosis (DVT), common signs are swelling, pain, warmth, and redness in a limb, often the calf. For pulmonary embolism (PE), look for sudden shortness of breath, chest pain, rapid heart rate, and coughing up blood. Arterial clots can cause stroke-like symptoms such as sudden weakness, confusion, or speech difficulties. It's vital to seek immediate medical attention if you suspect a clot.
How are blood clots treated?
Treatment typically involves anticoagulant medications (blood thinners) to prevent the clot from growing and to allow the body to dissolve it over time. In some severe cases, clot-dissolving drugs (thrombolytics) or surgical procedures to remove the clot may be necessary. The specific treatment depends on the clot's location, size, and the patient's overall health.
Can I prevent blood clots?
Yes, prevention is possible, especially for those at moderate risk. Key strategies include staying active, avoiding prolonged sitting or immobility, maintaining a healthy weight, not smoking, and staying hydrated. For individuals with higher risk factors, a doctor might prescribe preventative medications or recommend compression stockings. Regular exercise and movement are your best allies.
What is the difference between a thrombus and an embolism?
A thrombus is a blood clot that forms and stays attached to the wall of a blood vessel. An embolism occurs when a piece of a thrombus, or another substance like an air bubble or fat globule, breaks off and travels through the bloodstream, potentially lodging in a smaller vessel and causing a blockage elsewhere. A pulmonary embolism (PE) is a common example where a DVT breaks off and travels to the lungs.